A conference to help clinical staff in West Yorkshire to better identify and treat the life-threatening infection sepsis has been held in Leeds.
Sepsis can be hard to spot because there are a lot of possible symptoms, some which can be vague and some that can mimic other conditions like flu, diarrhoea or chest infections.
The conference, StampOutSepsis2, was the second free sepsis event organised by Leeds Teaching Hospitals Trust and focused on educating NHS teams from across the region by sharing the experiences of staff and sepsis survivors on topics that included recognising sepsis early, treating it promptly and understanding the support needed for those who have survived the infection.
In the UK it is estimated that there are around 50,000 deaths from sepsis every year – more than those who die from breast, bowel and prostate cancer combined – yet with early diagnosis it is easily treatable.
Dr Yvette Oade, Chief Medical Officer for Leeds Teaching Hospitals Trust, said the conference was to help staff across West Yorkshire become more familiar with the signs and symptoms of sepsis so they could provide swift treatment when suspicions are aroused.
“Acting quickly is important when sepsis is suspected as it gives patients a much better chance of survival,” she said. “We already have protocols in place in our hospitals but we felt it was important to share lessons learned across the Trusts in West Yorkshire so that we can all be better at spotting and dealing with sepsis for the benefit of patients.”
Among those who addressed the conference was sepsis survivor Molly Spencer, 12, from Tadcaster who was diagnosed with sepsis at the age of four after picking up an e-coli infection while on holiday in Northumberland.
She became very ill and needed kidney dialysis treatment, but her condition stabilised after treatment at Leeds General Infirmary and she eventually recovered but still needs check-ups every year.
Her mother, Julia, said it was a huge shock to see her daughter being struck down with what was originally thought to be a diarrhoea and vomiting bug, and end up in kidney failure within 48 hours.
“Events like the Leeds conference provide education and awareness of the signs and symptoms of sepsis and most importantly to empower everyone to ask, ‘Could this be sepsis?’,” she said. “The importance of early recognition and treatment is paramount in providing the best possible outcome for the patient.”
Another sepsis survivor who addressed the conference was Tom Ray, Nic Ray his wife and carer, and Pippa Bagnall, a clinician who presents with Tom and Nic.
Tom developed sepsis out of the blue in 1999. He deteriorated rapidly but the diagnosis of sepsis took nearly 24 hours. By then, the condition was so advanced he had to have both his arms and legs amputated to save his life and suffered facial disfigurement because of the infection.
“I want to share my experience of sepsis with as many people as possible,” he said. “By talking about what happened to me I hope it will save lives and help survivors.”
His wife Nic gave birth to their second child while Tom was in a four-month coma and said sepsis has a dramatic effect on the whole family. “From being a successful businesswoman I became a full time carer and mother to two little children. It was tough, but I wasn’t offered any help and I was unaware of what support existed,” she said.
Pippa Bagnall added: “Sepsis does not discriminate so the awareness challenge is massive. Tom and Nic share their story of surviving sepsis with humility, transparency and passion.
“We are delighted to be back in Leeds where there is clearly a huge commitment to tackling sepsis awareness.”
Leeds Teaching Hospitals Trust has already introduced the LEEDS observational sepsis screening tool in its Children’s Hospital:
● Look for sepsis
● Evaluate the risk of sepsis
● Escalate to a senior clinical decision-maker
● Diagnose risk of sepsis
● Start antibiotics within an hour if sepsis is likely
Dr Kerry Jeavons, a consultant paediatrician at Leeds Children’s Hospital, welcomed the conference and said it was important frontline staff, as well as families, were more aware of sepsis.
She said sepsis “champions” have been created on each ward in the Children’s Hospital and, this year, the LEEDS sepsis screening tool had been rolled out to use on all acute paediatric admissions and for any child who deteriorates on the wards.
“Children get infections and fevers a lot, which is a part of normal childhood, and the vast majority of these will make a prompt and full recovery,” she said.
“However, we strongly encourage families that if their child deteriorates, or they are still concerned, they should ask whether it could be sepsis and seek immediate medical advice.”
What Is Sepsis?
Sepsis is the immune system’s overreaction to an infection or injury. Normally our immune system fights infection – but sometimes, for reasons we don’t yet understand, it attacks our body’s own organs and tissues. If not treated immediately, sepsis can result in organ failure and death. Yet with early diagnosis, it can be treated with antibiotics.
Signs And Symptoms Of Sepsis
Adults:
● Slurred speech or confusion
● Extreme shivering or muscle pain
● Passing no urine (in a day)
● Severe breathlessness
● It feels like you’re going to die
● Skin mottled or discoloured
Children:
● Is breathing very fast
● Has a ‘fit’ or convulsion
● Looks mottled, bluish, or pale
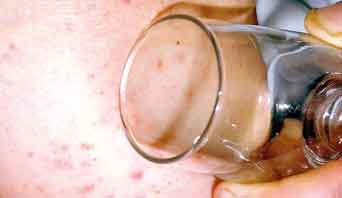
● Has a rash that does not fade when you press it
● Is very lethargic or difficult to wake
● Feels abnormally cold to touch